Polycystic Kidney Disease has plagued many families throughout the world, including my own. It often leads to kidney failure and a need for dialysis or transplantation. I was diagnosed with PKD at the age of 21 I never envisioned all that I would experience as life moved forward. This will be a journey of humor, sadness, desperation, love, frustration and all other emotions that come with spending a life bound to a machine you learn to love to hate keeping me alive. Blessings
Saturday, September 30, 2017
Wednesday, September 6, 2017
National Kidney Foundation "Disaster Preparedness"
https://www.kidney.org/sites/default/files/11-10-0807_IBD_disasterbrochure.pdf
EMERGENCY!! Home Dialysis Central article on Disaster Planning for Home Dialysis
Disaster Planning For PD And Home HD
Epic tornados. Earthquakes. Hurricanes. Tsunamis. Nuclear power plant meltdowns! It seems as if a good part of the news each day reports on a fresh disaster. No one wants to have to deal with events that disrupt vital services—like dialysis. But if life throws a fire storm or flood your way, you'll have a better chance of making it through if you prepare.
Gather Key Papers
In any type of disaster, you'll be a step ahead if you know where your vital documents are and can grab them in a hurry. Make a folder or binder with:

- Your health history, meds list, recent lab test results, and Advance Directive
- Insurance plan information (health, home or renter's, car)
- Phone numbers for loved ones, the power and water companies, your doctor(s), drugstore, and your dialysis clinic and backup clinic
- Proof of I.D. (copies of driver's license, passport, Medicare card, etc.)
- Bank and credit card information
- Home deed and car registration
Keep your folder in a safe place that will be easy to reach when you need it, like a nightstand, dresser drawer, or kitchen cupboard. You might even store it in a plastic Ziploc bag in the fridge. Update the contents as things change in your life. Always be sure your clinic knows how to reach you.
For the purpose of home dialysis, disasters fall into one of two types:
- You must stay at home (with or without power and water)
- You can't stay at home (you have to evacuate)
When You Must Stay At Home
 A pandemic flu, huge blizzard, or flood may keep you in your home and off the roads. If the power is on and you have PD or home HD supplies on hand—you're in luck! Being able to do your treatments at home in an emergency is one of the unsung benefits of home options. In the Kobe, Japan, earthquake of 1997, PD patients fared far better than those who were doing in-center HD. 1
A pandemic flu, huge blizzard, or flood may keep you in your home and off the roads. If the power is on and you have PD or home HD supplies on hand—you're in luck! Being able to do your treatments at home in an emergency is one of the unsung benefits of home options. In the Kobe, Japan, earthquake of 1997, PD patients fared far better than those who were doing in-center HD. 1Make An Emergency Kit
In a plastic bin, gather:
- Flashlight and batteries
- Weather band radio (a hand crank type won't need batteries)
- A week's supply of your meds
- A first aid kit
- Chemical hand warmers (be very careful about using these—they do get hot)
- Paper plates and cups, and plastic forks, knives, and spoons
- A scissors and knife
- A can opener
- Trash bags
- Bleach or iodine to purify water
For PD, you'll need to have these supplies: 2
- 5 cases of solution (1.5%, 2.5%, and 4.25%)
- Masks
- 1 case of lines and caps
- Betadine and hand sanitizer
- Extra batteries for your blood pressure monitor
For home HD, you'll need to have these supplies: 3
- 7 days of home HD supplies (If you use a NxStage machine with a PureFlow device, have backup bags on hand. Be sure they have not expired.)
- Nxstage cartridges or dialyzers and lines
- Saline bags
- Needles
- Tape and scissors
- Syringes and heparin
- Gloves and hand sanitizer
- Meds you use
 You may want to do treatments somewhat less often to stretch out your supplies, if you are not sure how long an emergency will last. If there is no water :
You may want to do treatments somewhat less often to stretch out your supplies, if you are not sure how long an emergency will last. If there is no water :- You can use hand sanitizer and do PD.
- You can do home HD with a NxStage machine and bags, but not with a standard home HD machine.
If there is no power :
- You can do PD by hand. You may want to have chemical hand warmers on hand to heat your bags. Ask your PD nurse if you could safely use these in an emergency, with a towel on top to protect the PD bags from the heat.
- You would need backup power to do home HD
Back-Up Light & Power
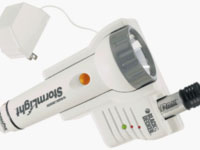 You're doing a home treatment at night and the power goes out. It's pitch dark! What do you do? We hope you think about this ahead of time and get an emergency light. These flashlights plug into a power outlet. When the power goes out, they come on. You can find these for under $25 online or in hardware stores, so you can see what you're doing for a safe disconnect for PD, or a manual rinseback for HD.* Or, keep a flashlight or camping lantern with fresh batteries in easy reach—just in case. A "headlight" type flashlight will leave your hands free. LED bulbs last longer than the standard ones.
You're doing a home treatment at night and the power goes out. It's pitch dark! What do you do? We hope you think about this ahead of time and get an emergency light. These flashlights plug into a power outlet. When the power goes out, they come on. You can find these for under $25 online or in hardware stores, so you can see what you're doing for a safe disconnect for PD, or a manual rinseback for HD.* Or, keep a flashlight or camping lantern with fresh batteries in easy reach—just in case. A "headlight" type flashlight will leave your hands free. LED bulbs last longer than the standard ones.
* When the power is out, the air detector on an HD machine will not work. Shine a flashlight on the blood tubing as you do a manual rinseback to be sure that you are not getting air in the lines. If you see bubbles, don't rinse back the blood. It's better to lose what's in the circuit than risk an air embolism.
 You can get short-term power (from 15 minutes to a few hours or so) from an uninterruptable power supply (UPS). Office supply stores carry these to prevent damage to computers. Hardware stores may have them, too. You plug a UPS into the wall, and plug your machine into the UPS. The battery in the UPS charges while the power is on. When the power goes out, the UPS keeps the machine running long enough for you to safely disconnect. The longer the back-up power, the more they cost—from a couple of hundred dollars to over $1000. So, if you go this route, you might think about how much time you would need to safely return your blood—not run a whole treatment.
You can get short-term power (from 15 minutes to a few hours or so) from an uninterruptable power supply (UPS). Office supply stores carry these to prevent damage to computers. Hardware stores may have them, too. You plug a UPS into the wall, and plug your machine into the UPS. The battery in the UPS charges while the power is on. When the power goes out, the UPS keeps the machine running long enough for you to safely disconnect. The longer the back-up power, the more they cost—from a couple of hundred dollars to over $1000. So, if you go this route, you might think about how much time you would need to safely return your blood—not run a whole treatment.
Someone at the store may be able to help you choose a UPS. You will need to know how many watts the machine uses (this should be in the manual or on the back of the machine, or you can call the company and ask them).
 If you really want to be self sufficient, you can get longer-term power from a generator that runs on gasoline (or propane, which is safer to store). You can't run a generator indoors. It could create a carbon monoxide build-up. Generators can also be quite noisy. So, you'd need a sheltered place outside to run it, and a long power cord to reach your machine. You'd also need a partner to plug in the generator for you if the power goes out during a treatment.
If you really want to be self sufficient, you can get longer-term power from a generator that runs on gasoline (or propane, which is safer to store). You can't run a generator indoors. It could create a carbon monoxide build-up. Generators can also be quite noisy. So, you'd need a sheltered place outside to run it, and a long power cord to reach your machine. You'd also need a partner to plug in the generator for you if the power goes out during a treatment.Emergency Food & Water Supply
 When you can do your treatments, you just need to have jugs of water, and food on hand that will not spoil. If you use canned or dried foods, you'll need to rotate them, since the shelf life is only about 6 months.
When you can do your treatments, you just need to have jugs of water, and food on hand that will not spoil. If you use canned or dried foods, you'll need to rotate them, since the shelf life is only about 6 months.
But...if you lose power, you may not be able to do your treatments. Or, you could run out of PD or home HD supplies. So, you need to have foods for the emergency dialysis meal plan that do not have to be cooked or kept cold. Your clinic can tell you about this plan, or it's in the Planning for Emergencies booklet from the National Kidney Foundation. 4
Coast Guard approved food bars have calories with very little salt, and a 3-day bar costs less than $4. The bars will keep for 5 years (look on Amazon.com). Talk to your dietitian. These bars would be boring to eat for days on end, but may be a good way to have a back up food supply that is safe for you with no dialysis.
Keeping In Touch With Loved Ones
In an emergency, phone lines may be down:
- If you can't leave your home, charge your cell phone while you have power, in case it goes out later.
- If there is a signal, call loved ones and they can tell others that you're okay—or pass along a message about what you need.
- Sometimes a text message will go through even if there is not enough of a signal for a call.
- Your land line phone may or may not work. If it doesn't, keep trying.
- While the power is on, you might try sending an email or a Facebook message.
When You Can't Stay At Home
 In some types of disasters, it is not safe for you to stay in your home. You must evacuate. You may have warning ahead of time—if a hurricane is coming, or forest fires are moving your way. Or, you may not have a lot of time to react. When you know ahead of time, try to get things ready:
In some types of disasters, it is not safe for you to stay in your home. You must evacuate. You may have warning ahead of time—if a hurricane is coming, or forest fires are moving your way. Or, you may not have a lot of time to react. When you know ahead of time, try to get things ready:- Fill up your car with gas, or make plans for how you'll get out. NOTE: In stop-and-go traffic, gas can run out quickly. Just 10 seconds of idling uses more gas than shutting off your engine.
- No car? Ask your clinic what type of transportation may be able to pick you up. Chances are, it will not be able to bring your dialysis supplies.
- Look at a map and work out a safe route. Bridges, trees, or power lines may be down.
- Gather your key papers, meds (or at least the empty bottles), some emergency food and water, a few days of PD or home HD supplies*, small valuables, cell phone and charger, and clothes.
- Load your car with the biggest items first, then the next biggest, and so on. Put small things in around big ones. This will let you fit more in. (You can fit more clothes in a suitcase by using the same tip.)
- Watch TV or listen to the radio to find out where the shelters are near you, or go on to another town. Your clinic may call and tell you where to go. 5
- Hide valuables you can't bring in unlikely places, like under clothes in a laundry hamper, in the veggie drawer of the fridge, or behind books in a bookcase. Lock all doors and windows to your home when you leave.
- Call your loved ones to tell them where you plan to go, or set up a meeting place. Again, text messages may work when phone calls do not. The American Red Cross Safe and Well List 6 on the web lets you tell your loved ones that you are okay.
- You can bring pets with you if you plan to leave town—but most shelters can't take them.
- If you go to a shelter tell the shelter staff that you are on dialysis when you arrive.
* If you can get to a town that is not part of the disaster, you can pick up new supplies at a dialysis clinic or have them shipped to you.
If you do PD and can't find a clean room for exchanges, don't do them . The risk of peritonitis is higher than the risk of not doing PD for up to a week. 1 Follow the emergency dialysis diet if you don't do your treatments. A red or sore exit site can be treated with a vinegar solution made in a very clean jar, with: 7
- 6 oz. (3/4 cup) boiled or bottled water
- 4 oz (1/2 cup) white vinegar
- 1 ¾ teaspoons table salt
Shake the jar until the salt dissolves and pour the solution into a clean spray bottle. It keeps for one week.
Spray on the vinegar after you clean your exit site with antibacterial soap and rinse off the soap. You can also soak a 4x4 gauze pad with the solution and lay it around your catheter for 20 minutes. It should feel soothing. If not, don't use it and seek medical attention.
Home Dialysis Emergency Resources
There are some very good emergency resources that can help you:
- The American Association of Kidney Patients has a free online service calledMy Health where you can enter your lab test results and health information—and then get to it from any computer with internet access.
- DaVita Patient Hotline: 800-400-8331.
- Fresenius Patient Hotline: 800-626-1297.
- The Kidney Community Emergency Response (KCER) Coalition has up to date information about emergencies. Visit kcercoalition.com, or call 1(813)-383-1530.
- The National Kidney Foundation has a free 40-page booklet called Planning for Emergencies: A Guide for People with Chronic Kidney Disease that you can download.
- NxStage offers a free 22-page disaster planning guide called Are You Ready? .
No one wants to have to deal with a disaster. But if one strikes, being ready ahead of time can make all the difference.
References:
- Sakai R. The Japanese experience during the Kobe earthquake: Management of continuous ambulatory peritoneal dialysis patients in a disaster. Renal Failure. 1997;19(5):693-99.
- Disaster preparedness for peritoneal dialysis patients. Florida Kidney Disease Coalition. Accessed 4/18/11.
- Are you ready? NxStage Home Hemodialysis Patient Planning Guidebook for Non-Medical Emergencies. Accessed 4/18/11.
- National Kidney Foundation. Planning for Emergencies: A Guide for People with Chronic Kidney Disease. Accessed 4/18/11.
- Kleinpeter MA, Norman LD, Krane NK. Disaster planning for peritoneal dialysis programs. Adv Perit Dial. 2006;22:124-9.
- American Red Cross Safe & Well List. Accessed 4/18/11.
- Centers for Disease Control and Prevention. Infection control for peritoneal dialysis (PD) patients after a disaster. Disaster Recovery Fact Sheet. Accessed 4/18/11.
Subscribe to:
Posts (Atom)